DETAILED INVESTMENT PROPOSAL: THE EECA LUNG HEALTH SOVEREIGNTY HUB
Catalyzing National Ownership, Political Certainty, and Regional Health Security in Eastern Europe and Central Asia
EXECUTIVE SUMMARY: INVESTING IN A SELF-RELIANT HEALTH FUTURE WITH POLITICAL CERTAINTY
The Eastern Europe and Central Asia (EECA) region stands at a defining point. Faced with persistent lung health epidemics, escalating geopolitical complexities, and a fundamental shift in global health financing, the imperative for national ownership and regional self-reliance in health has never been more pronounced. This Detailed Investment Proposal outlines a strategic opportunity to support the EECA Lung Health Sovereignty Hub, a Minimum Viable Product (MVP) requiring an initial investment of $1,000,000. This Hub is designed to be a powerful catalyst for political will, community empowerment, and data-driven policy reform, specifically tailored to navigate this new, challenging global health landscape.
Crucially, the Hub is not a nascent endeavor. It builds upon the established, high-impact infrastructure and deep relationships of the Global TB Caucus, active in the EECA region since 2014. This existing network, comprising nine active national caucuses (Armenia, Azerbaijan, Georgia, Kazakhstan, Kyrgyzstan, Moldova, Tajikistan, Ukraine, Uzbekistan), provides a strong foundation for rapid, sustainable impact. By strategically leveraging AI technology as an enabling tool within this robust political and civil society architecture, the Hub will also function as a Health Security Coordination Center, ensuring continuity of care and integrated assistance for vulnerable patients even amidst active conflict or severe geopolitical events. This proposal details a lean, high-impact pathway to strengthen health sovereignty, regional resilience, and sustainable lung health systems across EECA, offering national donors a strategic, measurable, and timely investment in the region's health and stability, providing politicians with increased certainty in their decision-making.
1. THE OPPORTUNITY: A NEW ERA OF HEALTH FINANCING AND REGIONAL IMPERATIVES
The EECA region is currently navigating a set of complex health, economic, and geopolitical challenges that demand a strategic and localized response.
1.1. The Global Fund Transition: A Call for National Ownership
Beginning with the 2026–2028 allocation cycle, the Global Fund is progressively reducing its financial and operational footprint in several countries in the EECA region, as part of its broader strategy to prioritize settings with higher disease burden and lower income—a trend further reinforced by a more constrained replenishment. This evolving funding landscape is creating significant financing gaps and underscores the urgent need for EECA countries to strengthen sustainable, domestically financed health systems. International donors are increasingly advocating for national ownership and the development of robust local funding mechanisms, placing the onus on regional advocates to secure and optimize internal resources [1, 2]. This transition presents a unique opportunity for national donors to step forward and champion a model of self-reliance.
1.2. Persistent Lung Health Crises
The EECA region bears one of the world's highest burdens of tuberculosis, with 18 high-priority countries accounting for approximately 85% of the TB burden and 99% of the multidrug-resistant TB (MDR-TB) burden [3]. Other lung health conditions, such as chronic respiratory diseases and emerging respiratory infections, further strain already fragile health systems. These persistent challenges demand innovative, efficient, and locally-driven solutions.
1.3. Geopolitical Instability and Health Security
Escalating geopolitical instability and security issues across the region underscore the urgent need for resilient health systems and strategic autonomy in essential medical supplies. The decline in global health donor spending further exacerbates this vulnerability. In the event of conflicts or geopolitical events, the Hub's proposed role as a Health Security Coordination Center becomes paramount, ensuring uninterrupted, coordinated assistance to all affected patients, irrespective of the prevailing security situation. This is a direct investment in regional stability and human security.
1.4. Inefficient Resource Allocation and Data Gaps
Despite increasing health expenditures in many EECA countries, budgets are often misaligned with actual disease burden due to fragmented planning, limited health spending intelligence, and insufficient forecasting. The promise of data-driven health is immense, but it is often hampered by incomplete Civil Registration and Vital Statistics (CRVS) systems, fragmented facility reporting, and a lack of interoperable health information systems. Without robust data governance, standards, and privacy safeguards, the potential of digital health remains untapped, risking donor skepticism about "AI breakthroughs."
2. THE SOLUTION: THE EECA LUNG HEALTH SOVEREIGNTY HUB (MVP)
The EECA Lung Health Sovereignty Hub is designed as a lean, high-impact Minimum Viable Product (MVP), strategically focused on catalyzing political will, community empowerment, and data-driven policy reform within a $1,000,000 budget. Our approach is built on the principle of regional ownership and sustainability, leveraging existing strengths and addressing critical gaps.
2.1. Building on Established Foundations: The Global TB Caucus Network
Unlike new initiatives that require extensive foundational work, the Hub benefits from the pre-existing, robust infrastructure of the Global TB Caucus. This network has been actively engaged in the EECA region since 2014, cultivating strong relationships and a proven track record of mobilizing political commitment for lung health. The Hub will directly integrate and amplify the work of nine active national Global TB Caucuses in Armenia, Azerbaijan, Georgia, Kazakhstan, Kyrgyzstan, Moldova, Tajikistan, Ukraine, and Uzbekistan. These established relationships provide an unparalleled platform for rapid engagement and impact, significantly reducing start-up time and costs [4].
2.2. Lean, Autonomous Regional Governance Structure
The Hub will operate as an autonomous, regionally-led center, ensuring that decisions are made by and for the EECA context, while remaining strategically connected to the broader Global TB Caucus network. This lean structure is designed for agility, direct impact, and fostering regional ownership and accountability. It avoids bureaucratic overhead, allowing for efficient allocation of the $1,000,000 MVP budget directly to programmatic activities.
Governance Model:
- Regional Steering Committee: Composed of representatives from the Parliamentary Council, Civil Society Council, and key technical experts from the region. This committee will provide strategic direction, oversight, and ensure alignment with regional priorities.
- Parliamentary Council: Drawing directly from the active national Global TB Caucuses (Armenia, Azerbaijan, Georgia, Kazakhstan, Kyrgyzstan, Moldova, Tajikistan, Ukraine, Uzbekistan), this council will champion legislative and policy reforms, advocate for domestic resource mobilization, and ensure political buy-in at the highest levels. Their established relationships and influence are critical for translating policy into action.
- Civil Society Council: Comprising representatives from affected communities and civil society organizations across the EECA region, this council will ensure that the Hub's activities are community-led, rights-based, and responsive to the needs of vulnerable populations. It will provide ethical oversight, particularly for data use, and ensure accountability and transparency.
- Expert and Alumni Platform: This platform brings together former Members of Parliament, regional champions, and technical experts with longstanding experience in lung health. It will serve as a strategic advisory and advocacy network, offering institutional memory, mentorship, and continuity of engagement beyond electoral cycles. The platform will support high-level advocacy, facilitate peer exchange, and help sustain political momentum on TB by leveraging trusted voices and established expertise across the region.
- Secretariat: A small, agile team responsible for day-to-day operations, technical support, and efficient implementation of the MVP pillars.
2.3. The $1M MVP: Focused Pillars for Political Certainty and Rapid Impact (12-Month Demonstrator)
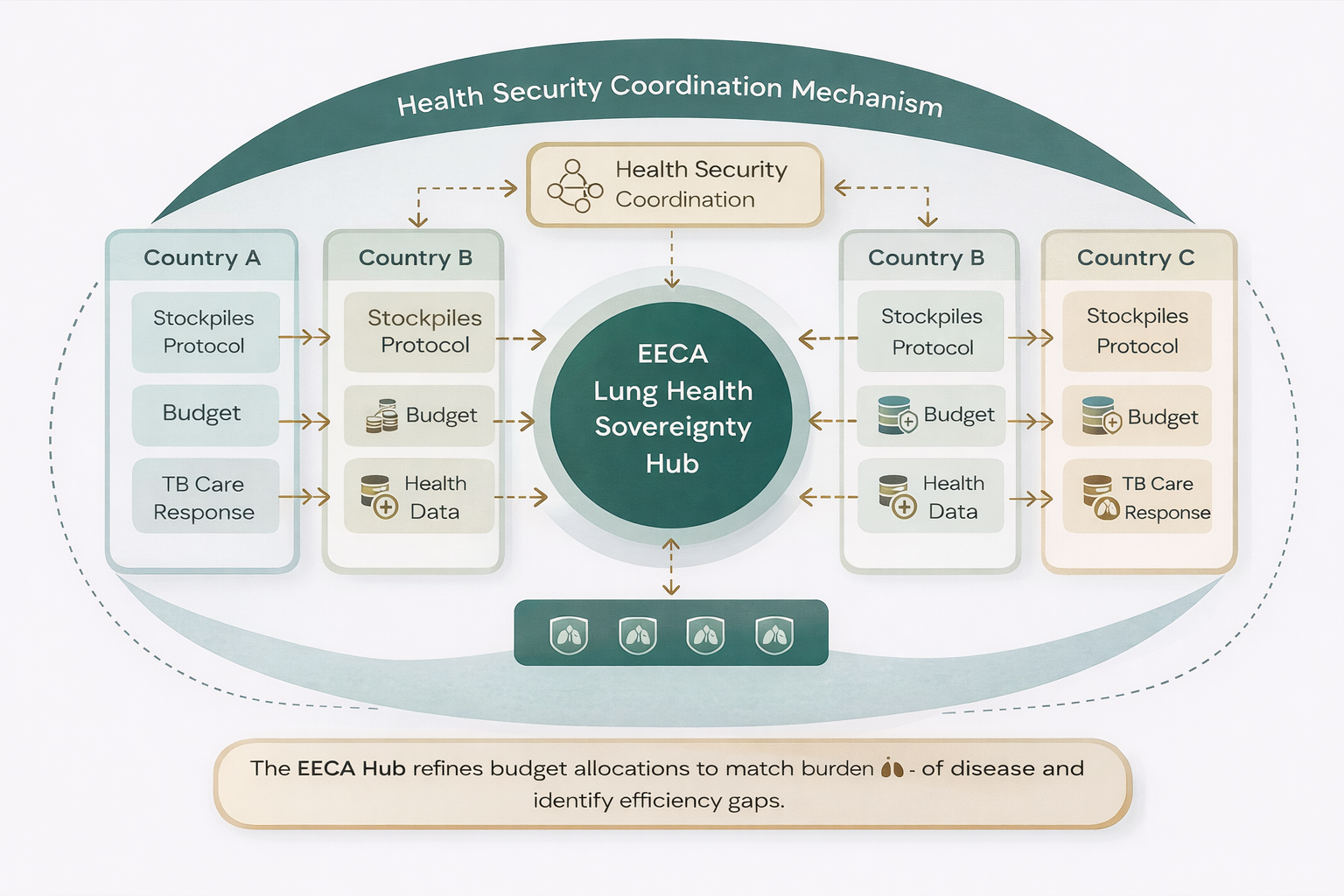
The MVP is designed to deliver high-impact, decision-relevant outputs within a lean $1,000,000 budget. It focuses on a limited number of pilot countries (2–3) and prioritizes tangible results over large-scale infrastructure. The Hub operates through three tightly integrated pillars and a cross-cutting coordination function. Together, they form a single decision-support system that connects financing, operations, and accountability into a coherent, usable mechanism for governments and partners.
3. THE INVESTMENT THESIS: HIGH-LEVERAGE, RAPID IMPACT FOR NATIONAL DONORS
This $1,000,000 MVP offers national donors a high-leverage investment in a practical, results-oriented model that delivers tangible outputs within 12 months. The Hub is designed to improve how financing decisions are made, how health systems are monitored and coordinated, and how accountability is ensured. The model focuses on a limited number of pilot countries and a defined set of decision-support outputs that can be demonstrated, validated, and scaled. It directly supports governments, parliaments, and partners in navigating the transition toward more domestically financed and operationally resilient health systems.
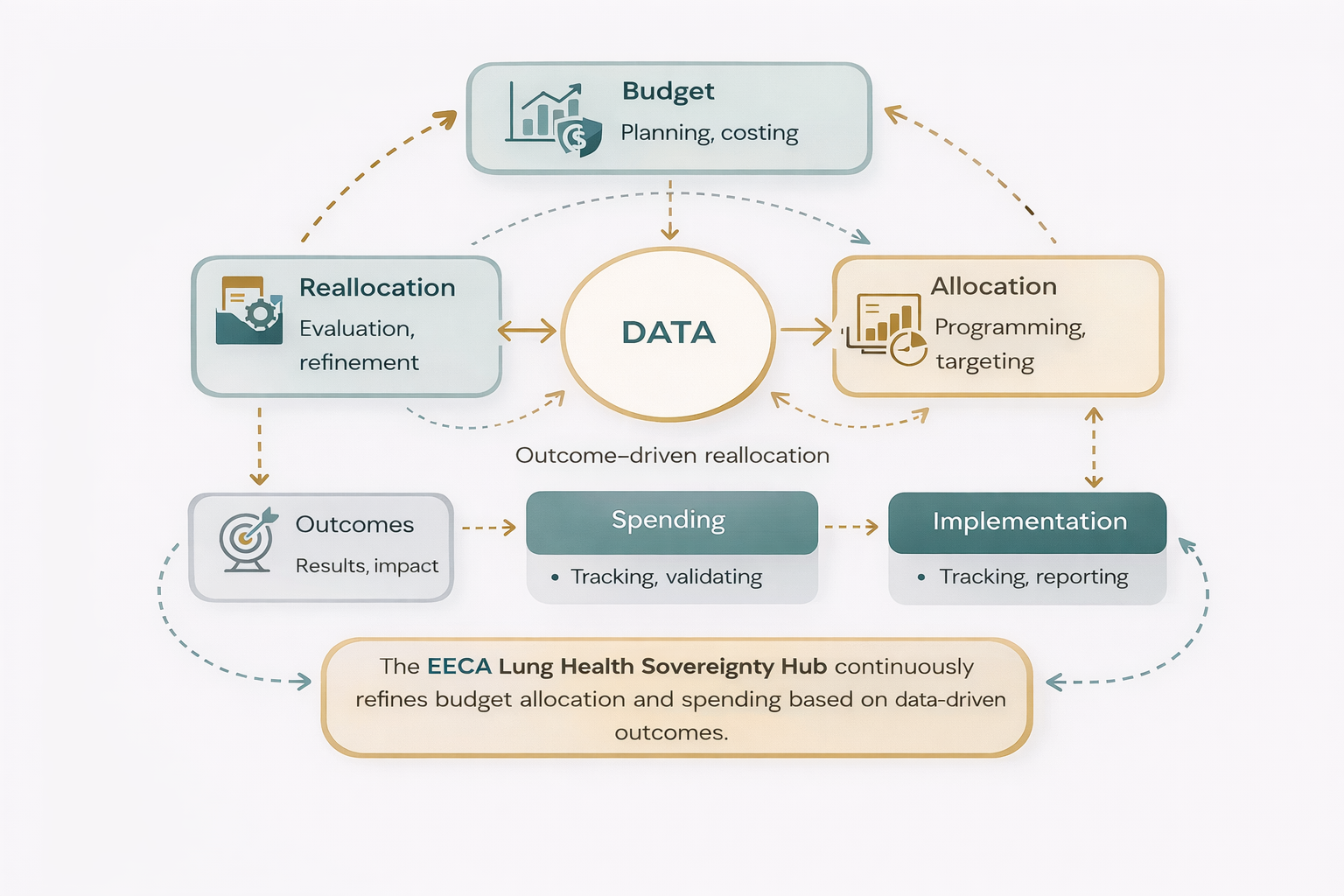
3.1. Pillar 1: Budget and Policy Intelligence – Improving Financing Decisions
This pillar addresses a core structural gap in the region: the lack of clear, actionable insight into how health resources are allocated, and how policy decisions translate into financial commitments. It supports governments in aligning spending with disease burden, system needs, and fiscal realities. By building on the established Global TB Caucus network, the Hub leverages existing political relationships to ensure that financial and policy analysis is directly connected to decision-making processes, rather than remaining purely technical [4].
Why it's investable for national donors: This pillar strengthens national capacity to manage and optimize domestic health financing. It helps governments reduce inefficiencies, prioritize high-impact interventions, and make more realistic policy commitments in the context of donor transition. By linking financial analysis to parliamentary processes, it increases the likelihood that evidence is translated into actual budget decisions.
Impact: Decision-makers receive Budget Review Reports, Resource Mapping Analyses, Policy Costing Models, and Spending Alignment Recommendations that clarify how resources are currently used and how they can be improved. Legislative and Budget Impact Notes provide structured input into policy discussions, enabling more informed and financially grounded decisions.
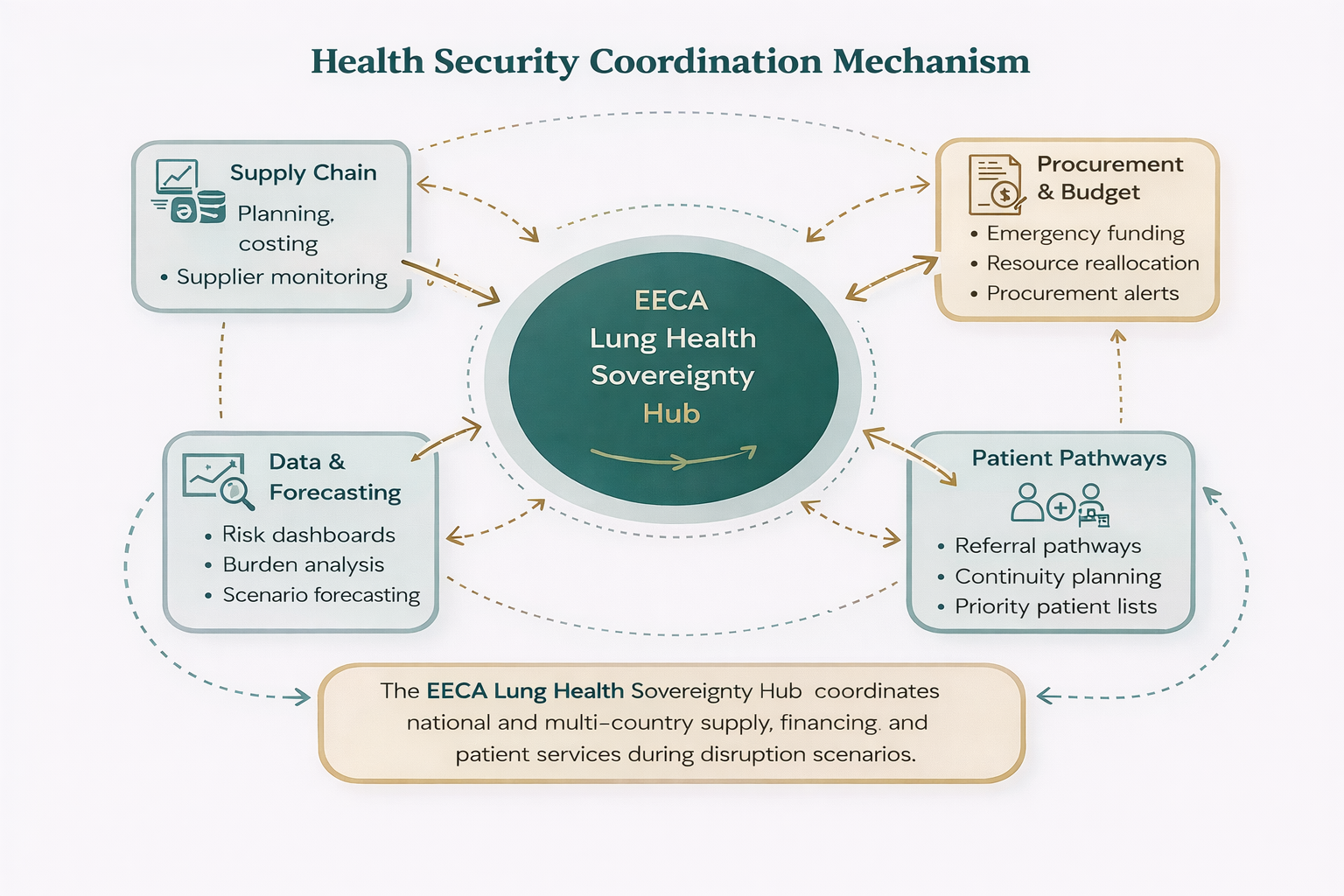
3.2. Pillar 2: Operational Intelligence and Health Security – Planning, Forecasting, and Continuity
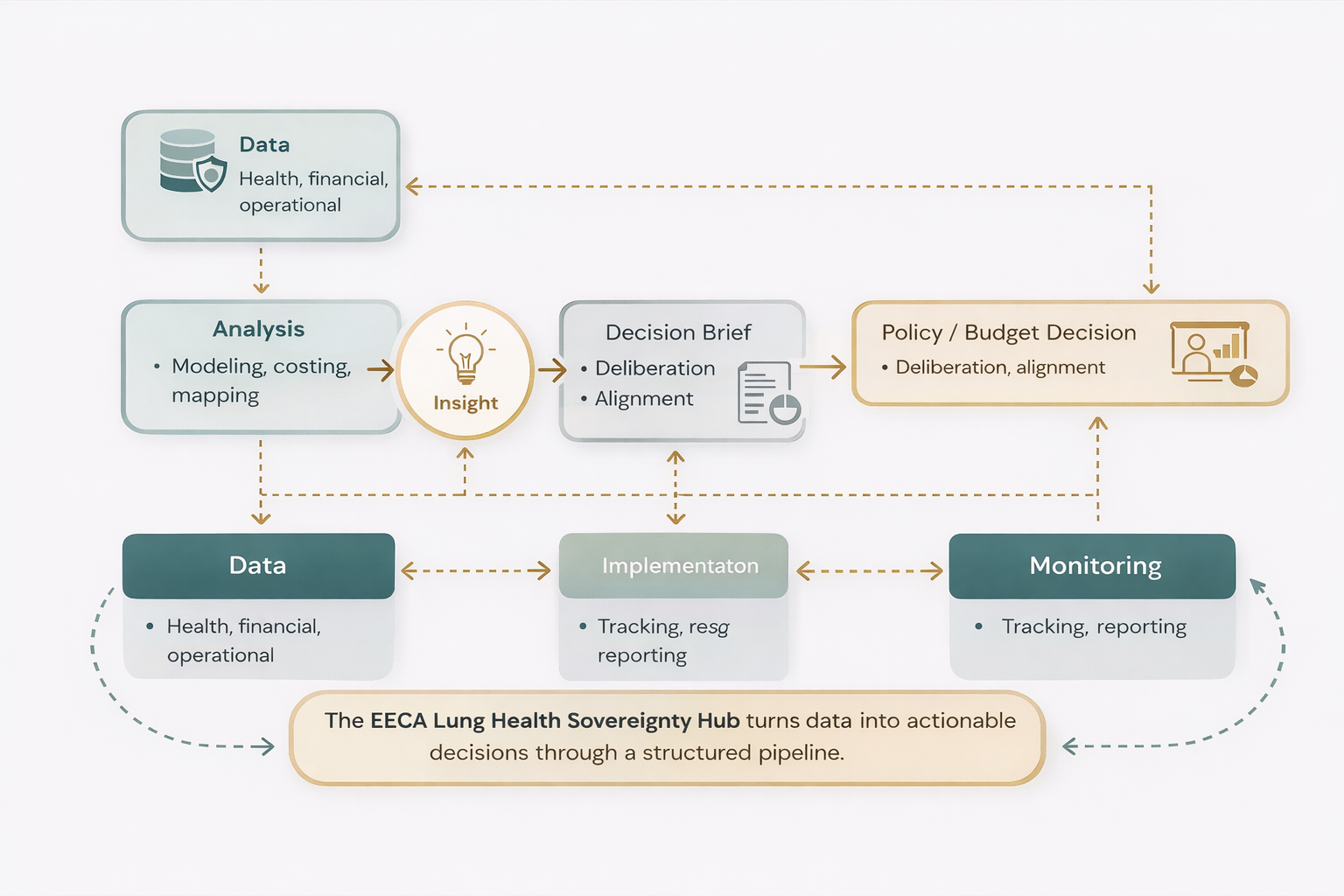
This pillar establishes a practical operational intelligence function that transforms fragmented data into usable insight for planning, forecasting, and continuity of care. It focuses on building concrete tools—dashboards, analytical models, forecasting systems, and decision briefs—that support both routine management and response to disruption. AI is applied selectively to clearly defined analytical tasks: forecasting resource needs (e.g. drugs, diagnostics, service demand); identifying inefficiencies in spending relative to disease burden; synthesizing multi-source data into structured decision outputs. These functions are implemented within a governed system, ensuring usability, transparency, and alignment with real decision-making processes.
Why it's investable for national donors: This investment strengthens national capacity to monitor system performance, anticipate operational risks, and make coordinated resource decisions. It provides governments and partners with practical tools that improve planning, procurement, and continuity of care, while avoiding reliance on complex or costly infrastructure [5].
Impact: Decision-makers gain access to interactive dashboards, burden-versus-spending analyses, AI-supported forecasting models, and decision briefs. These outputs improve visibility of system performance, enable earlier identification of risks, and support more coordinated responses in both stable and disrupted contexts.
3.3. Pillar 3: Parliamentary and Public Accountability – Ensuring Follow-Through and Transparency
This pillar ensures that financing and policy decisions are not only made, but tracked, debated, and followed through. It focuses on strengthening parliamentary engagement, oversight mechanisms, and structured dialogue between government, civil society, and technical actors. By building on the Global TB Caucus network, the Hub anchors accountability within existing parliamentary structures while expanding the tools available for monitoring and engagement [4].
Why it's investable for national donors: This pillar increases transparency and accountability in the use of public resources. It strengthens the link between allocation and implementation, ensuring that funding decisions translate into real outcomes. This contributes to greater public trust and more effective use of national budgets, which is essential in contexts of constrained financing and increasing demand for efficiency [6].
Impact: Through caucus engagement frameworks, budget advocacy toolkits, oversight and monitoring systems, and accountability scorecards, stakeholders are able to track decisions over time and ensure implementation. Structured dialogue mechanisms create continuous feedback between policymakers, implementers, and communities, reinforcing accountability and improving system performance.
4. BUDGET ALLOCATION (APPROXIMATELY $1,000,000 MVP)
The $1,000,000 MVP budget is structured to support delivery of a focused 12-month programme across 2–3 pilot countries. It prioritizes analytical outputs, pilot implementation, stakeholder coordination, and lightweight operational systems over large-scale infrastructure. The budget is designed to be realistic for a small technical secretariat working through existing regional networks, while ensuring sufficient resources for country-level engagement, production of decision-support outputs, and cross-cutting governance and coordination.
This budget is designed to be highly efficient, focusing on tangible outputs and leveraging the established networks to achieve significant results within a short timeframe.
5. POTENTIAL RISKS AND MITIGATION STRATEGIES
While the EECA Lung Health Sovereignty Hub is designed to strengthen regional ownership and sustainability, several risks may affect implementation during the initial phases. The initiative incorporates mitigation measures to reduce these risks and ensure adaptive implementation.
6. CONCLUSION: A STRATEGIC INVESTMENT IN NATIONAL HEALTH AND REGIONAL STABILITY
The EECA Lung Health Sovereignty Hub, with its $1,000,000 MVP, offers a strategic, high-impact investment opportunity for national donors. By focusing on activating political will through the established Global TB Caucus model, building community-led data governance with responsible AI, optimizing resource allocation for lung health, and critically, serving as a Health Security Coordination Center during times of regional instability, we will demonstrate rapid, measurable progress towards a more resilient and sovereign health landscape in the EECA region. This MVP is not just a project; it is a proof-of-concept for a new era of intelligent, community-driven health investment that prioritizes patient well-being, national economic stability, and regional security above all else. We invite you to partner with us in securing the health future of the EECA region.
REFERENCES
- Human Rights Watch. Donor Nation Cuts to Global Health Financing Affect Millions. January 22, 2026. https://www.hrw.org/news/2026/01/22/donor-nation-cuts-to-global-health-financing-affect-millions
- Impakter. Individual American Donors Are Shifting to Domestic Needs. November 26, 2025. https://impakter.com/individual-american-donors-are-shifting-to-domestic-needs-implications-for-philanthropy/
- World Health Organization. Global Tuberculosis Report 2023. https://www.who.int/teams/global-tuberculosis-programme/tb-reports/global-tuberculosis-report-2023
- Global TB Caucus. https://www.globaltbcaucus.org/
- World Health Organization. WHO global strategy on digital health 2020-2025. https://www.who.int/docs/default-source/documents/gs4dh-final-web.pdf
- Gavi, the Vaccine Alliance. Gavi's Strategy for 2026-2030 (Gavi 6.0). https://www.gavi.org/our-alliance/strategy/gavi-6-0